How Gastric Bypass Surgery Is Performed
The Roux–en–Y gastric bypass (RGB) is the most common weight-loss surgery procedure and combines two approaches. First, a small pouch is created by stapling the stomach, reducing the amount of food it can hold. Next, a Y–shaped section of the small intestine is surgically attached to the pouch in order to allow food to bypass the upper and lower sections of the small intestine. This reduces how much the digestive track can absorb of the food and nutrients that have been consumed.
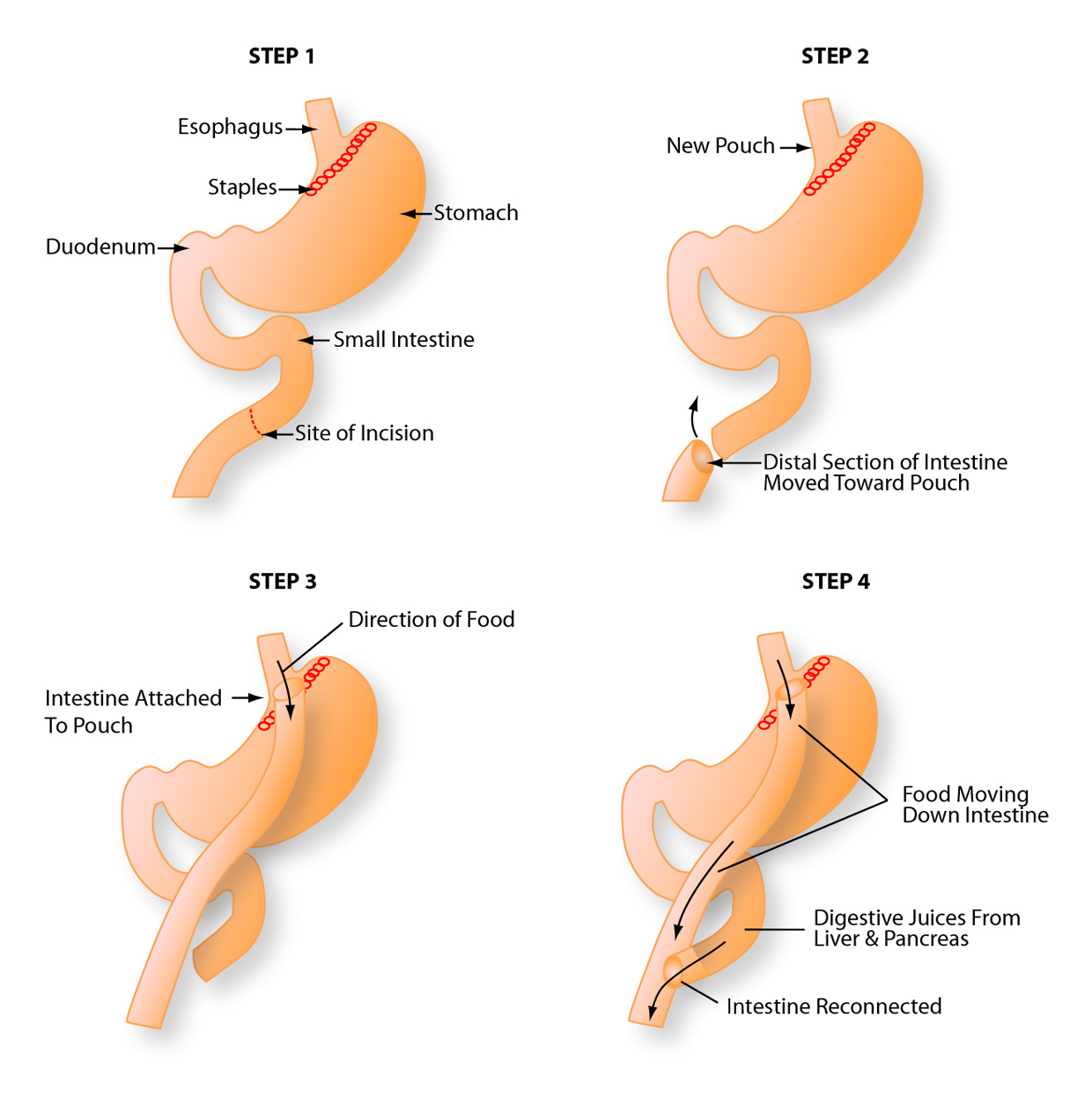
Gastric bypass operations that restrict food intake and cause malabsorption result in more weight-loss than those operations that only restrict food intake. Patients who have bypass operations generally lose two–thirds (80%) of their excess weight within two years.
The gastric sleeve surgery can be performed robotically. Using the latest robotic surgical system, our surgeons have improved visualization, dexterity, precision and control, while only making small 1-2 cm incisions. Our patients often experience less pain and scarring, shorter hospital stays, and a quicker recovery to normal activity.
Potential complications associated with these procedures may include a response called “dumping syndrome” — nausea, cold sweats, rapid heart beat, dizziness and possible diarrhea — which can be brought about by certain foods such as those that are high in fat or refined sugar; enlargement of the pouch caused by consistent overeating, resulting in inadequate weight loss or regaining some weight; nutritional deficiencies caused by bypassing the duodenum, where most iron and calcium are absorbed, requiring lifetime vitamin supplements; anemia brought about by malabsorption of Vitamin B12 and iron in menstruating women, and decreased absorption of calcium may induce osteoporosis and metabolic bone disease. The more extensive the bypass operation, the greater the risk for complications and nutritional deficiencies.