Aortic Dissection
Aortic dissection is a tear in the wall of the aorta that causes blood to flow between the medial layers of the wall of the aorta and force the layers apart. Aortic dissection is a medical emergency. If the dissection tears through all three layers of the aorta, massive and rapid blood loss occurs.
Acute vs. chronic
If the symptoms or dissection occur within the last 14 days, the dissection is termed acute aortic dissection. If the symptoms or dissection occur after the 14th day, the dissection is termed chronic aortic dissection.
Complicated vs. un-complicated
The term “complicated” aortic dissection is used for patients who present with, or during the hospital course, develop the following: rupture, malperfusion syndromes (poor blood supply to the intestine, kidneys or legs), refractory pain or rapid aortic expansion. This is an important distinction as patients with complicated aortic dissection usually require endovascular or open surgical intervention.
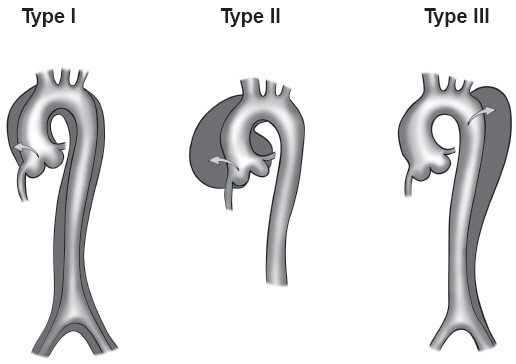
The DeBakey classification
The DeBakey classification of aortic dissection: Type I refers to dissections that propagate from the ascending aorta, extend to the aortic arch, and commonly, beyond the arch distally. Type II refers to dissections that are confined to the ascending portion of the aorta. Type III dissections are limited to the descending aorta. Class III also includes the dissections that start in the descending aorta that extends proximally to the arch and ascending aorta.
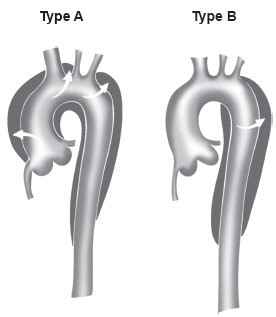
The Stanford classification
The Stanford classification of aortic dissection: Stanford Type A includes aortic dissections that involve the ascending aorta (with or without involvement of the transverse and descending thoracic aorta). Stanford Type B includes aortic dissections that originate in the descending (and thoracoabdominal) aorta, regardless of any retrograde involvement of the arch.